 Confidential
Confidential  Safe
Safe  Fast
Fast










get tested, know your status
What is OraQuick In-Home HIV Test and how does it work?
The OraQuick In-Home HIV Test is a rapid self-administered over-the-counter (OTC) test and tests for HIV in oral fluid. This test works by looking for your body’s response (antibodies) to fighting the HIV virus. A positive result is preliminary, and follow-up testing is needed.
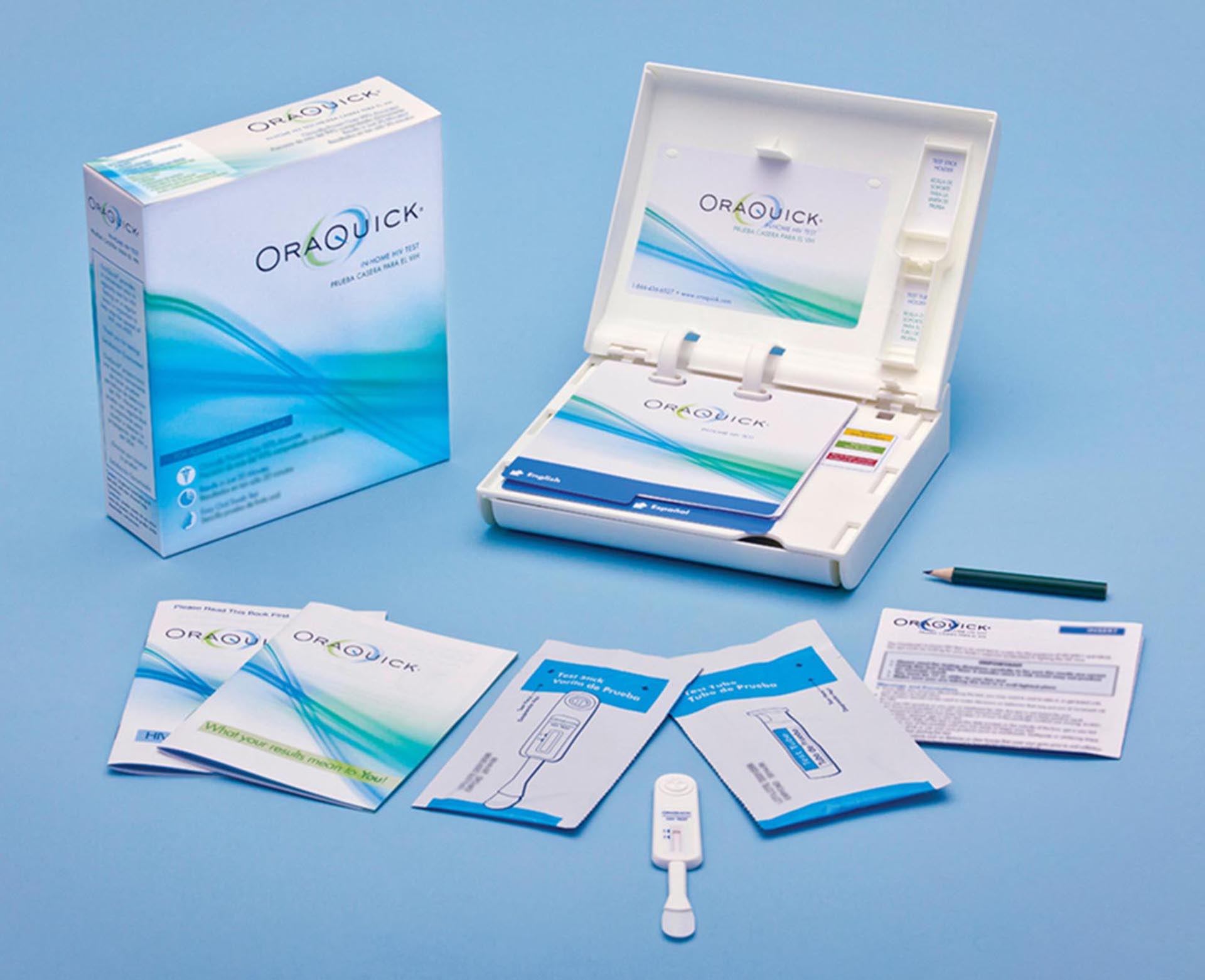
What is included?
The OraQuick In-Home HIV Test kit consists of:
Testing Directions
A Disposal Bag
Phone Numbers For Testing Support
A Single Use Test Stick (Device) To Collect The Specimen
A Single Use Test Tube (Vial) Prefilled With 1mL Of Developer Solution
Wo Information Booklets (“HIV, Testing And Me” And “What Your Results Mean To You”)
How do I perform the test?
The OraQuick test package contains step-by-step instructions and it is extremely important to carefully read and follow all labeled directions. The kit is designed to allow HIV testing to be done anonymously and in private. To perform the at home test:
- Use the test stick (device) and swab the upper and lower gums.
- Insert the test stick (device) into the kit’s test tube (vial) which contains a developer solution.
- Wait 20-40 minutes before you read the test result.
If any piece of the test kit is missing or appears to have been opened, do not use the test and contact the OraQuick Support Center toll free at I -866-436-6527.

How do I perform the test?
As noted in the package insert, clinical studies have shown that the OraQuick In-Home HIV Test has an expected performance of approximately 92% for test sensitivity (i.e., the percentage of results that will be positive when HIV is present). Even when used according to the labeled directions, there will be some false negative results and a small number of false positive results.
A positive result with this test does not mean that an individual is definitely infected with HIV but rather that additional testing should be done in a medical setting to confirm the test result.
A negative test result does not mean that an individual is definitely not infected with HIV, particularly when exposure may have been within the previous three months.
It can take some time for the immune system to produce enough antibodies for the test to detect, and this time period can vary from person to person. This timeframe is commonly referred to as the “window period,” when a person is infected with HIV but antibodies to the virus cannot be detected, however, the person may be able to infect others. According to the Centers for Disease Control and Prevention, although it can take up to 6 months to develop antibodies for HIV, most people (97%) will develop detectable antibodies in the first 3 months following the time of their infection.










